Navigating Autism
About 1 in 54 children in the U.S. has been diagnosed with autism spectrum disorder (ASD), according to estimates from the CDC’s Autism and Developmental Disabilities Monitoring (ADDM) Network.[1] Getting an ASD diagnosis is a life-changing event for families that can trigger feelings of panic, fear and distress. You may be uncertain or confused about what to do next and how to navigate your new reality. Here are tips to help you and ensure your child lives their best life.
Do your homework—Learn everything you can about ASD and how it may affect your child throughout their life, including the laws and rights that you and your child have under the Individuals with Disabilities Education Act. The knowledge you gain will help you be an effective advocate for your child.
Become a voice for your child—As a parent, you are your child’s first, strongest and lifelong advocate. No one knows your child better than you do. You are the best qualified person to shape your child’s situation in the most caring way and speak out when it comes to their well-being and ensuring that they have the supports they need to flourish.
Seek help—The autism community is full of parents and professionals willing to help others in their ASD journeys. Allowing others to help can lighten your load, help you become a better advocate and protector for your child, and make the sometimes difficult journey more enjoyable. Seek out support groups, teachers, therapists, social workers and others for help.
Give help when you can—If you can, helping other parents on their ASD journeys can help you to put things in perspective, feel more positive about your own circumstances and create a sense of belonging. Helping others has shown to lower levels of stress and anxiety, which improves overall well-being.
Express yourself—As human beings, we need connection. Sharing your feelings with someone you trust, such as your partner or spouse, parents and/or siblings, can be liberating and go a long way in deepening your relationships, and improving your physical and mental well-being, making you a better person, parent and family member.
Make self-care a priority—Spending most of your time caregiving can quickly lead to burnout. Proper hydration, a healthy diet and sufficient sleep can help you cope best with daily challenges. Finding time for activities that are fun and fulfilling, such as going to the gym, going for walks and meeting friends, can help you recharge and be the best parent you can be.
Find the right providers—While it is important that your child’s providers use evidence-based practices and keep abreast of treatment options, it is also important that they are culturally aware and respect your ideas and traditions. Each cultural group has its own customs, thoughts and taboos regarding physical and mental health care. Find a doctor who not only speaks your language, but is also sensitive to your cultural, religious and personal beliefs.
Foster healthy eating habits—Children with ASD often experience issues such as insomnia, eczema, constipation, diarrhea, behavioral outbursts and more. If your child has any of these issues, you might want to see if it is a reaction to foods that are not good for their system or if their intestines are out of balance. Healthy eating habits can make a big difference in the lives of children with ASD.
Nurture your child’s strengths—Children improve faster when they work on strengths. Focusing on your child’s strengths, not weaknesses, puts them on the path to their personal best, allows them to develop and excel in things they’re good at, and can greatly improve their self-esteem and well-being. It can also foster a better parent-child relationship.
Magellan Healthcare is committed to improving all lives affected by autism. Visit our Autism Awareness website here for free resources that increase awareness, celebrate differences and support inclusion.
Read more Autism content from Magellan Health Insights
[1] https://www.appliedbehavioranalysisedu.org/top-10-awesome-things-about-being-on-the-autism-spectrum/
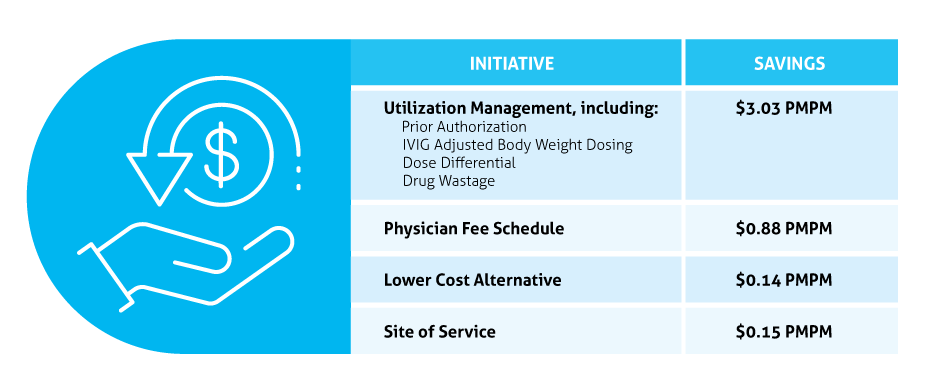
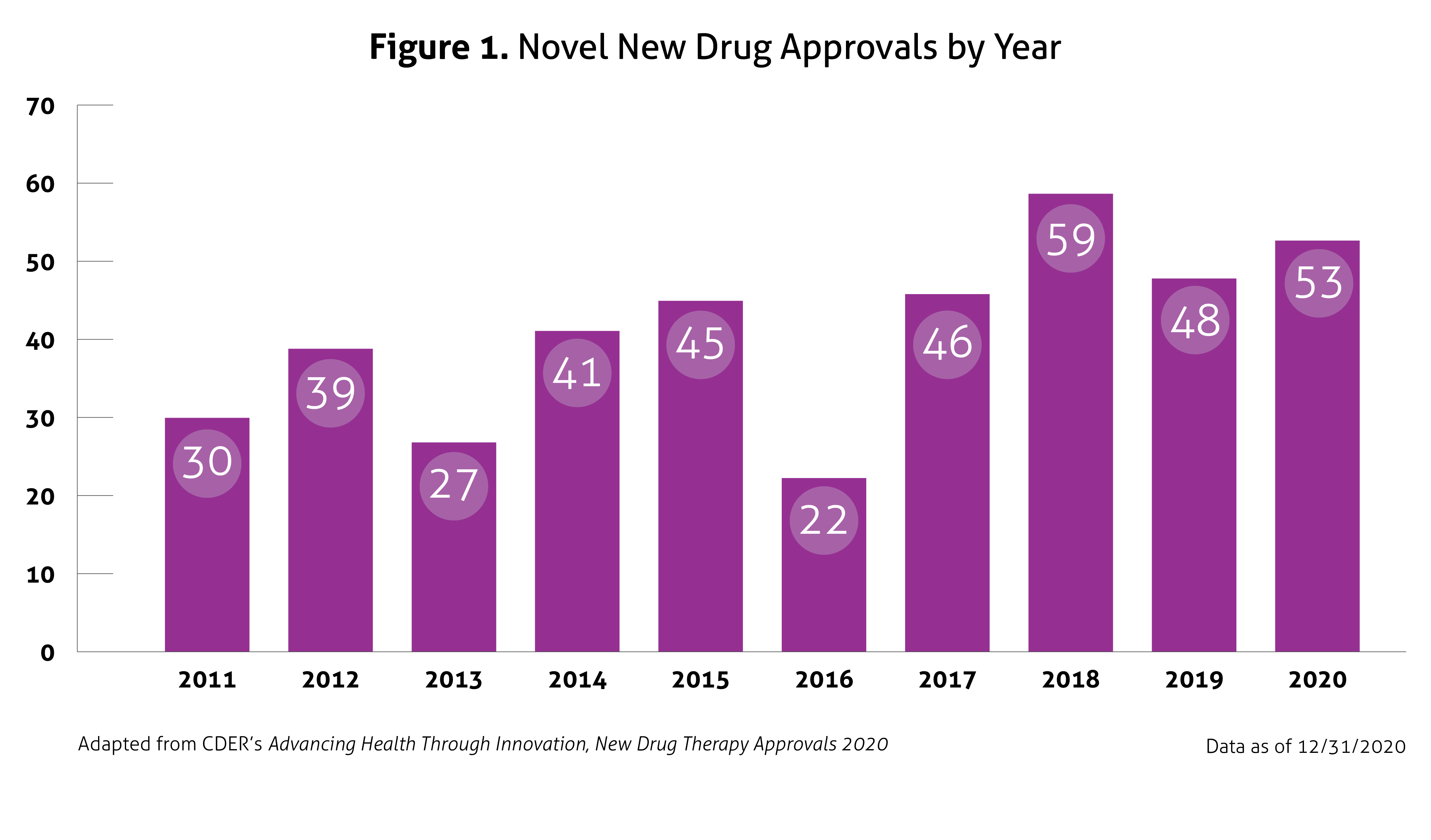 Despite the ongoing pandemic the FDA continued their strategic initiatives to expedite the safe review of treatments in 2020. With the unprecedented challenges incurred in 2020, the FDA acknowledged that maintaining their commitment to bringing forth innovative therapies was difficult. Remarkably, the numbers reported by the FDA do not include the several emergency use authorizations (EUAs) issued by the FDA for COVID-19.
Despite the ongoing pandemic the FDA continued their strategic initiatives to expedite the safe review of treatments in 2020. With the unprecedented challenges incurred in 2020, the FDA acknowledged that maintaining their commitment to bringing forth innovative therapies was difficult. Remarkably, the numbers reported by the FDA do not include the several emergency use authorizations (EUAs) issued by the FDA for COVID-19.